The “Freeze-or-Faint” Reflex: A Case of Panic-Induced Vasodepressive Syncope and Postural Tachycardia
A 35-year-old female was coming complaining of episodes of palpitation, dizziness and syncope that injured her twice in the last 2 weeks.
She describes that these attacks were triggered by emotional stress and for a less extent by orthostatic changes.
The patient consumes a large amount of caffeine, she does not smoke and has no medical history of importance.
Her resting blood pressure is 110/80 mmHg, her erect blood pressure dropped to 100/60 mmHg with marked increase in heart rate from 80 to 110 bpm with slight dizziness
Her echocardiography was normal, her labs did not show any abnormalities of concern with even normal cortisol levels, metanephrins and thyroid functions
She admits drinking less water than expected and she refused to decrease her caffeine consumption
She had a lot of medical advice with a lot of functional assumptions, crude nonprofessional reassurance and no improvement and no serious workup
We advised her to drink 3 liters per day, give her ivabradine to decrease heart rate and a follow up period of 1 month
Patient came with more episodes of syncope, obvious panic attacks and no improvement of her symptoms. This pattern rose the possibility of exaggerated vasodepressive syncope triggered by her emotional conditions
These complex loops are common in emotionally vulnerable patients
The relationship between vasodepressive (vasovagal) syncope and panic attacks is a frequent point of clinical overlap, often leading to diagnostic confusion because both involve the autonomic nervous system. However, they represent two fundamentally different directions of physiological response.
1. The Physiological “Fork in the Road”
While both conditions are triggered by stress or anxiety, they act on the Autonomic Nervous System (ANS) differently:
- Panic Attack (Sympathetic Overdrive): This is a “Fight or Flight” response. The sympathetic nervous system floods the body with catecholamines (epinephrine/norepinephrine), leading to tachycardia, hypertension, and hyperventilation. You feel like you are “speeding up.”
- Vasodepressive Syncope (Parasympathetic Overdrive): This is often a “Fainting” response. After an initial sympathetic surge, the body overcompensates with a massive vagal (parasympathetic) discharge. This causes a sudden drop in blood pressure (vasodepression) and/or heart rate (cardioinhibition), leading to cerebral hypoperfusion and loss of consciousness.
2. Key Clinical Distinctions
In your practice, differentiating these is vital for patient reassurance. Patients with panic attacks often fear they will faint, but they rarely do because their blood pressure is actually elevated.
Feature | Vasodepressive Syncope | Panic Attack |
Heart Rate | Brachycardia (Slows down) | Tachycardia (Races) |
Blood Pressure | Hypotension (Drops) | Hypertension (Rises) |
Skin Appearance | Pallor (Pale), Diaphoresis (Cold sweat) | Flushing or Tremor |
Loss of Consciousness | Yes (Brief) | Rarely (Usually “lightheadedness” only) |
Recovery | Rapid once horizontal | Gradual (10–30 minutes) |
3. The “Vasovagal Panic” Loop
There is a subset of patients where the two conditions coexist in a feedback loop:
- The Trigger: A patient experiences a mild physical sensation (like heat or a needle prick).
- The Panic: The patient interprets this sensation as a threat, triggering a panic attack (Sympathetic surge).
- The Reflex: The body reacts to the high heart rate and forceful contractions (Bezold-Jarisch reflex) by abruptly switching to a vagal response.
- The Syncope: The blood pressure bottoms out, and the patient faints.
4. Psychological Impact
For many, the fear of fainting again creates “anticipatory anxiety,” which can trigger a panic attack in situations where they previously fainted (e.g., a crowded mall or a clinic). This creates a cycle where the psychological state (panic) creates the physiological environment for the reflex (syncope).
5. Management Implications
As a cardiologist, you likely see these patients when they are referred for “blackouts.”
- Beta-Blockers: While used for some syncopal triggers (as discussed previously for HOCM or LQTS), they can sometimes be counterproductive in pure vasodepressive syncope if they worsen bradycardia. However, they can be useful in patients whose syncope is triggered specifically by the initial sympathetic surge of a panic attack.
- Tilt Table Testing: This remains the gold standard to see if a patient’s “panic” sensation actually leads to a measurable drop in BP/HR.
- Counter-pressure Maneuvers: Teaching patients to tense their leg muscles can physically prevent the vasodepressive drop during a panic-induced prodrome.
On the Diagnostic Overlap & Autonomic “Switching”
These studies examine how the brain’s “threat response” can trigger the Vasovagal reflex.
- D’Alessio, S., et al. (2024). “Autonomic Signature of Panic Disorder and its Overlap with Vasovagal Syncope: A Systematic Review.” Journal of Clinical Autonomic Research.
- Key Finding: Explores the “Sympathetic-Parasympathetic Switch,” where the initial tachycardia of a panic attack triggers the Bezold-Jarisch reflex, leading to sudden vasodepression.
- Raj, V., et al. (2023). “Psychiatric Comorbidities in Patients with Recurrent Syncope: The Role of Anxiety and Somatization.” Circulation: Arrhythmia and Electrophysiology.
- Key Finding: Highlights that up to 40% of patients with recurrent VVS meet the criteria for an anxiety or panic disorder, suggesting that psychological distress is a “primer” for the reflex.
2. On the Psychological Triggers of the Vasodepressive Response
These references focus on how the fear of fainting creates a physiological environment for syncope.
- Yasa, E., et al. (2022). “Anxiety and Depression in Patients with Vasovagal Syncope: A Case-Control Study.” Frontiers in Cardiovascular Medicine.
- Key Finding: Demonstrates a direct correlation between the frequency of syncopal episodes and the severity of panic-related symptoms, emphasizing the “Anticipatory Anxiety” loop.
- Atici, A., et al. (2023). “The Impact of Panic Attacks on the Yield of Tilt-Table Testing.” International Journal of Cardiology.
- Key Finding: Shows that patients with comorbid panic disorder have a lower threshold for a “positive” (fainting) response during Head-Up Tilt Testing (HUTT).
3. On Management (The “Crossover” Treatments)
These papers discuss how treating the anxiety/panic component can reduce the cardiac syncopal events.
- Buszko, K., et al. (2023). “Pharmacological Management of Recurrent Vasovagal Syncope: Focus on SSRIs and Beta-Blockers in High-Anxiety Populations.” Current Cardiology Reports.
- Key Finding: Reviews why Selective Serotonin Reuptake Inhibitors (SSRIs) are often more effective than traditional cardiac drugs for patients whose syncope is triggered by panic.
- Jandackova, V. K., et al. (2022). “Heart Rate Variability as a Biomarker of Panic-Syncope Interaction.” Psychosomatic Medicine.
- Key Finding: Uses HRV (Heart Rate Variability) to map how the “Fight or Flight” response collapses into a “Freeze or Faint” response.
Summary Table for Clinical Use
Study Focus | Primary Mechanism Identified | Clinical Takeaway |
D’Alessio (2024) | Sympathetic-to-Vagal Switch | Panic can “force” a vasodepressive event. |
Raj (2023) | Comorbidity Prevalence | High anxiety lowers the syncopal threshold. |
Buszko (2023) | SSRI Efficacy | Treating the mind can stabilize the heart’s reflex. |
On this background we advised her to seek psychological help and to perform a tilt table test to confirm the vasodepressive syncope
The psychiatrist confirmed the panic attacks and the deep depression the patient suffer due to social major problems
On the other hand, the tilt table test became positive
So, the patient was given on tip of her ivabradine a combination of Citalopram 10 mg and midodrine 25 mg three times per day
This new treatment with improving hydration served on decrease her dizziness, stopped her syncopal attacks and decreased the episodes of panic attacks she has
This case highlighted the importance of integrating the psychological with organic or pathological mechanisms in patients’ complaints, diagnostic workup and management
To terminate or not to terminate?
That is the question!
By: Ghada Youssef, MD
A 32-year-old lady, Gravida 2, para 2, with a history of 2 cesarean section deliveries (which were both uneventful), and not a known hypertensive, diabetic or a smoker.
She was presented to the Pregnancy-Heart team at the High-Risk Pregnancy Unit on her 35th week gestation with persistent BP of 160/100 mmHg and sinus tachycardia at a rate 95 bpm. She was diagnosed as HDP (Hypertensive disorder in pregnancy). The patient was admitted to hospital for frequent BP follow up and other investigations were ordered. She was prescribed Labetalol 100 mg bid and Alpha methyl Dopa 250 mg tds and her BP was closely monitored in hospital.
Laboratory findings included: Hb=7 g/dL (hypochromic, microcytic), PLT=85,000/HPF, AST=244 mg/dL, ALT=270 mg/dL, Creatinine=0.9 mg/dL, Albumin=2.4 mg/dL, Proteins in urine= 3 g/24hours, BNP=693 pg/dL.
ECG and fundus examination were normal, and echocardiography showed the following: LVEDD: 5.4 cm, LVESD: 3.3 cm, LVEF: 66%, SWT: 1.1 cm, PWT: 1.0 cm, LA: 3.8 cm and grade 1 diastolic dysfunction.
Based on these investigations, the patient was diagnosed as preeclampsia with severe manifestations and HELLP syndrome.
Obstetric evaluation to the fetus showed absence of signs of maturity.
**In this situation, what would be your decision?
1- Terminate pregnancy immediately.
2- Wait till BP control.
3- Wait for labour pains to begin.
4- Council the patient and wait for 2 more weeks.
As her gestational age was 35 weeks on presentation, the decision was to terminate pregnancy immediately by CS delivery. Her baby was incubated for 2 weeks and was discharged afterwards.
After delivery: her laboratory tests were back to normal after 2 days, her BP dropped to 140/90 mmHg, Alpha methyl Dopa was stopped, and Labetalol dose was reduced to 100 mg qd.
Follow up BP: after 1 month (BP 130/70 mmHg) and Labetalol was discontinued, after 2 months (BP 110/80 mmHg) and after 3 months of delivery BP was 120/70 mmHg.
What do we learn from this case?
– Preeclampsia with severe manifestation is a serious disease that needs hospital admission and close BP and laboratory monitoring.
– Preeclampsia with HELLP syndrome in a pregnant lady with gestational age >34 weeks warrants termination of pregnancy.
– Preeclampsia can recur in a subsequent pregnancy, the incidence is 18%.
– Preeclampsia runs in families, so pregnant ladies with a positive family history of preeclampsia should be closely monitored throughout pregnancy till delivery and after delivery.
– Females with history of preeclampsia have a high incidence of HTN and cardiac diseases later in life, that is why annual assessment of cardiovascular risk is recommended.
Hypertension Case Studies
Mohsen Ibrahim, MD
A female patient with recent severe Hypertension
74 years old female referred because of history of recent severe HT and epistaxis. Two days before her clinic visit while visiting her husband in ICU she stumbled and bled from her nose. BP checked at that time was 220/? mmHg, she was given IV and sublingual medicine and left the hospital with BP 170/90 mmHg though epistaxis continued. On her first clinic visit, epistaxis stopped but she wanted to be reassured regarding her BP. She had no specific complaints except worrying about her husband who had a recent MI and she mentioned that she is under severe stress, and she was in good health before the last event. She was not known to be hypertensive with no history of antihypertensive drug intake or other medication except vitamins and had no family history of HT. she had no history of renal problems, operations, weight changes, intake of pressor medications (NSAIDS). During examination she looked depressed with mild skin pallor, her body weight was 74 kg and height 162cm BP measured supine several times ranged 208/124-180/118 mmHg, heart rate was 128 b/m and regular. Physical examination was unremarkable with intact peripheral pulsations and absence of cardiac or abdominal murmurs. ECG showed sinus tachycardia at a rate of 130 b/m and left atrial abnormality.
Laboratory tests were ordered and the patient was prescribed the following medications and sent home: Bisoprolol 5 mg BID, amlodipine 10 mg.
Valsartan 10 mg combination, torsemide 10 mg, SSRI (faverin 50 mg) and Zolam 0.25 mg.
Next day afternoon, a phone call from her daughter who mentioned that her mother was sleepy all day and her BP was 102/70-104/78 mmHg. She was asked to discontinue faverin and torsemide and to see her after 10 days.
Laboratory tests showed a blood urea of 85mg/dL, creatinine 1.3 mg/dL, uric acid 7.2 mg/dL, K 4.4 mmol/L, HB 11.8 mg/dL with normal blood sugar, TSH and lipid profile.
When patient was seen in her second clinic visit few weeks later, she was symptom free, BP was 164/100 mmHg, her ECG showed frequent PACs, LAE and possible LVH ( R in AVL = 12 mm). treatment was modified to bisoprolol 10 mg, plus a polypill of thiazide / amlodipine/ valsartan 160 mg.
Few weeks later the patient reported through a phone call she is symptom free, her home BP readings 140/80-165/95 mmHg. However her repeat laboratory tests showed a blood urea of 93 mg/dL, creatinine of 1.7 mg/dL while her optic fundus showed atherosclerotic changes and cotton wool exudates.
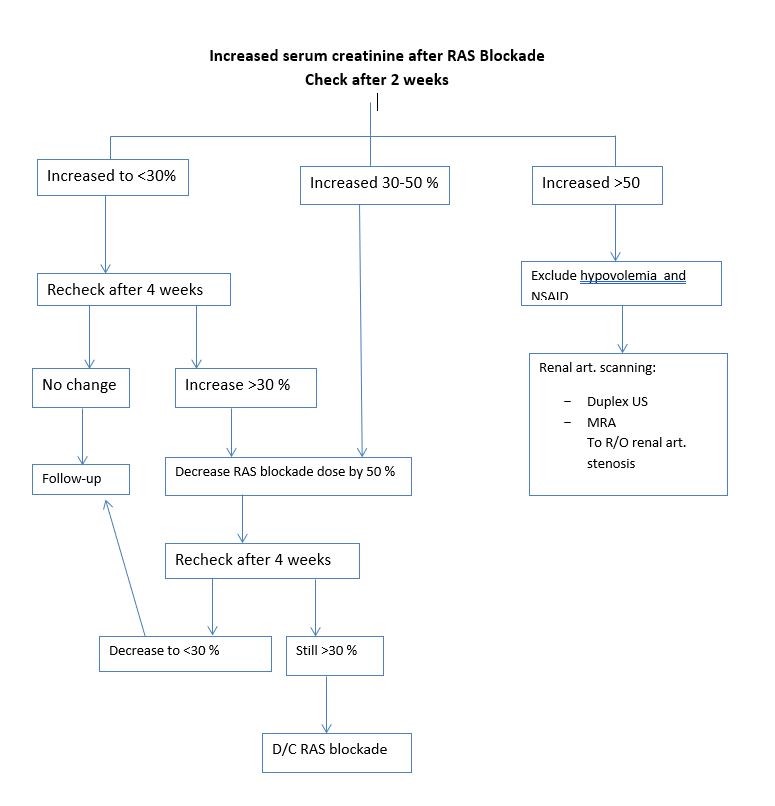
This acute rise in serum creatinine following RAS blockade was alarming. However it is normal up to 30 % of baseline level. However, if there is an increase more than 50% one has to exclude severe hypovolemia, NSAIDs intake, renal artery stenosis, polycystic kidney disease, sepsis or the use of cyclosporine.
On third office visit two months later, patient was symptom free, her home BP readings were 110/70 mmHg, BP at office was 144/90 mmHg, patients was asked to continue same treatment and recheck her serum creatinine and urea which turned out to be elevated . Creatinine was 1.9 mg/dL and urea 106 mg/dL, potassium 4.7 mg/L.
It was decided to discontinue valsartan and to refer the patient for renal artery duplex ultrasound which showed right renal artery stenosis.
Comments:
Clinical findings associated with renal artery stenosis:
Abrupt onset of HT at or after the age of 50 years.
Accelerated or malignant HT.
Refractory HT not responding to therapy with ≥ 3 drugs
Azotemia induced by treatment with RAS blocker.
Unilateral small kidney.
Unexplained hypokalemia
Abdominal bruit or over the flanks.
Severe retinopathy
Unexplained congestive heart failure or acute pulmonary edema
Vascular studies to evaluate the renal arteries:
Duplex ultrasonography: shows renal arteries and measures flow velocity
Magnetic resonance angiography: shows renal arteries and peri renal aorta . It is not nephrotoxic and is useful in patients with renal failure
Computed tomographic- angiography: shows renal arteries and peri renal aorta while providing excellent images. However, the large volume of contrast medium required is potentially nephrotoxic.
Renal artery stenosis
– May occur alone (isolated) or in combination with HT (reno-vascular or essential HT) or renal insufficiency (ischemic nephropathy) or both.
– In patient with renal artery stenosis and HT, HT is seldom cured by revascularization, except in those with fibro muscular dysplasia. Renal revascularization may improve and stabilize renal function in patients with renal artery stenosis and chronic renal failure.
– There is unproven benefit of renal revascularization compared with best medical therapy in atherosclerotic reno vascular disease.